A new CDC study found that some elderly people who apparently recovered from the coronavirus later came down with a second, even worse case — indicating that asymptomatic or mild cases may not provide a lot of protection against becoming reinfected with Covid-19.
The study, published Thursday in the Centers for Disease Control and Prevention's Morbidity and Mortality Weekly Report, studied two separate outbreaks that occurred three months apart at a skilled nursing facility in Kentucky. Between mid-July and mid-August, 20 residents and five health-care personnel tested positive for the virus, according to the study.
The second outbreak, between late October and the beginning of December, was worse — 85 residents and 43 health-care personnel tested positive for the virus. Among the residents who tested positive during the first outbreak and were still living in the facility, five of them tested positive a second time more than 90 days after their first positive test.
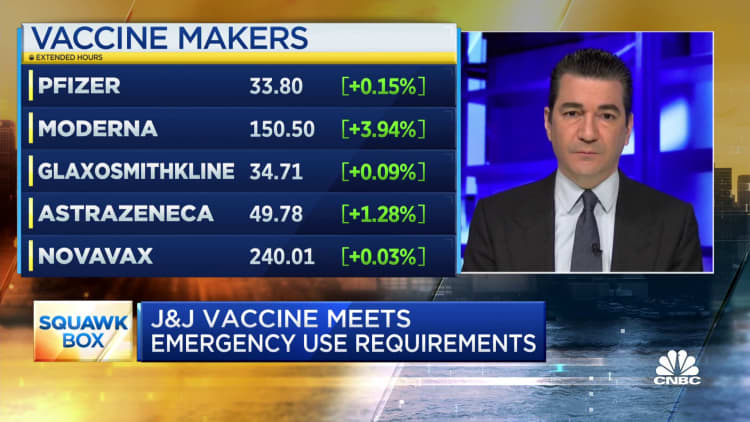

Though Covid-19 reinfections do happen, they are generally rare.
Through frequent surveillance after the first outbreak, all five residents had at least four negative tests between outbreaks, suggesting they were potentially reinfected with the virus later on, the study found. Reinfection means that a person who had Covid-19 recovered and then got it again, according to the CDC.
"The exposure history, including the timing of roommates' infections and the new onset of symptoms during the second outbreak, suggest that the second positive RT-PCR results represented new infections after the patients apparently cleared the first infection," wrote Alyson Cavanaugh, one of the researchers who led the study.
While only two of the five residents experienced slight symptoms during the first outbreak, all five potentially reinfected residents showed signs of illness the second time. The two residents who reported symptoms during the first outbreak "experienced more severe symptoms during the second infectious episode," according to the study. One resident was hospitalized and subsequently died.
According to the study's researchers, this was "noteworthy" because it suggests the possibility that people who show mild to no symptoms during their first infections "do not produce a sufficiently robust immune response to prevent reinfection." The results "suggest the possibility that disease can be more severe during a second infection."
"The findings of this study highlight the importance of maintaining public health mitigation and protection strategies that reduce transmission risk, even among persons with a history of COVID-19 infection," Cavanaugh wrote.
The study noted some limitations. Because specimens were not stored, researchers couldn't conduct genomic sequencing, a laboratory technique that breaks down the virus's genetic code, to confirm reinfection, researchers said. Also, "no additional test results exist to support the initial test result as a true positive" during the first outbreak, they said.
It's thought that the risk of reinfection for the general population is still low, but nursing home residents may be particularly at risk given their congregate living and high number of exposures, according to the study.
"Skilled nursing facilities should use strategies to reduce the risk for SARS-CoV-2 transmission among all residents, including among those who have previously had a COVID-19 diagnosis," Cavanaugh wrote.