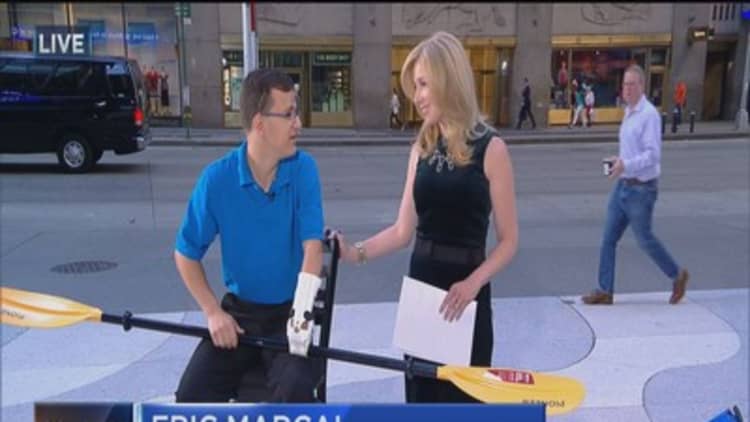
A year and a half ago, Dr. Albert Chi, a surgeon at the Johns Hopkins Hospital and an expert in prosthetic devices, was talking to a group of parents whose children suffered from congenital limb loss. He told them that prices don't make it feasible to fit children with advanced prosthetic devices — kids will outgrow them in months, and more money will have to be spent upsizing a prosthetic hand or limb. That's when one parent challenged Chi: Hadn't he heard of 3-D printing?
Within a month, Chi and the hospital found out about and began working with Enabling the Future, a network of volunteers across the world who 3-D-print prosthetic hands and fingers for children for free. Since the group's founding in 2013 by Jon Schull, a research scientist at the Rochester Institute of Technology, it has made more than 1,500 plastic hands for kids. At his lab at the Johns Hopkins Hospital, Chi fits patients for hands and creates those hands using three desktop 3-D printers he has available.
"People all over send us pictures of a hand next to a ruler; we scale the hand, and then we'll print them the proper size," he said. "Everything is printed — there's nothing metal in the hand at all."
Ushering in a new era of medicine
Additive manufacturing, generally referred to as 3-D printing, usually involves layering extruded thermoplastic or using a laser to transform a powdered metal or liquid resin into a three-dimensional object. Large manufacturing companies use additive manufacturing to construct prototypes or end-use parts, but over the last half decade, hobbyists and those new to 3-D printing have gained greater access to the technology, thanks to the proliferation of desktop 3-D printers.
Now 3-D printing is poised to usher in a new frontier in medicine, where the toxicity of drugs can be tested on living human tissue instead of animals, and personalized treatments are delivered to patients.
The prospects for the technology are strong. Over the next 10 years the industry is poised to boom. A report from IDTechEx estimates the global 3-D printing market will be $7 billion by 2025, with about half coming from 3-D bioprinting.
Read MoreA 3-D replica of your own organs
"There aren't necessarily things going into people's bodies," said Danny Cabrera, CEO of Philadelphia-based bioprinting start-up BioBots. "But we're using 3-D printing for a variety of different applications."

For instance, instead of relying solely on MRI and CT scans, surgeons are now able to print accurate replicas of patients' internal organs prior to surgery and simulate complicated surgeries beforehand, guiding their surgical teams through the steps needed to be taken later in the operating room. This new process increases the likelihood of a successful surgery.
Read MoreHow 3D printing will radically change the world
And while 3-D-printed complete organs ready for transplant are a decade away, at least, there have been examples of 3-D-printed structures serving as bone replacements. In the Netherlands in 2014, doctors replaced much of a patient's skull — which was slowly thickening and causing her headaches and vision loss — with a 3-D-printed plastic one. In September of this year, doctors in Spain implanted into a cancer patient a 3-D-printed titanium sternum and rib cage, snug substitutes for bones the patient lost when doctors excised a tumor.
Manufacturing human tissue
Perhaps more life-changing are the implications of the technology at the cellular level. Bioprinting, as it's called, usually involves mixing human stem cells, water and biocompatible material to produce living human tissue that can be matured into different types of human tissue — skin, liver, kidney, cartilage and so on.
This is the part of the field that Cabrera and co-founder Ricardo Solorzano's start-up — BioBots — has targeted: A BioBot is a desktop 3-D bioprinter, a machine about the size of a '90s computer monitor capable of printing living human cells and tissue. With a price tag under $10,000, it's much easier for researchers to procure a BioBot of their own. One researcher at Drexel University, for example, is using a BioBot in her lab to try to print bone tissue.
Bioprinting also opens up new ways of producing prescription pills. In August the Food and Drug Administration approved the first prescription drug developed via 3-D printing — a seizure medication for people with epilepsy, called Spritam, developed by Aprecia Pharmaceuticals. It was created from a set of biochemical inks, which means doses of the drug can be customized for each drug recipient.
And bioprinting allows for testing drug therapies on more than just animal cells.
"People have failures when they look at liver toxicity, because rat models aren't perfectly predictive," said Keith Murphy, CEO of California-based bioprinting company Organovo, which has been bioprinting liver tissue that can be used to test the safety and efficacy of certain drugs in treating liver diseases. "What we're able to show, so far, is we've been highly predictive of the true, eventual human impact of those drugs."
In April, Organovo signed deals with Merck and L'Oreal to share its 3-D-printing technology for the creation of skin and other types of cells.
Perhaps more life-changing are the implications of the technology at the cellular level. Bioprinting, as it's called, usually involves mixing human stem cells, water, and biocompatible material to produce living human tissue.
Of course, engineered cells and tissue created in a laboratory by means other than 3-D printing have already been put in patients, but completing that process by way of 3-D printing would not only ensure more precision and reproducibility but also provide a means to use a patient's own cells in the engineering of tissue.
"When we started 10 years ago, we were using a modified desktop printer. It worked, but it didn't have the right structural integrity where we could implant those tissues into patients," said Dr. Anthony Atala, director of the Wake Forest Institute for Regenerative Medicine. Today, using 3-D printers and bio-inks developed at Wake Forest, Atala and others are able to 3-D-print tissues and structures, like blood vessels, with the right rigidity for implantation and the automation necessary to scale up bioprinting so that it touches more patients.
"3-D printers are really just a way to automate the process [of creating human tissue] and increase the number of patients that can benefit from the technology," Atala said.
—By Andrew Zaleski, special to CNBC.com




